One Day in an LI Maternity Ward
Fathers separated from mothers.
Empty waiting rooms.
New parents testing positive for coronavirus.
How life begins under COVID-19.
Manuel Carchipulla watched with tears in his eyes as his wife, Diana Garcia Garcia, gave birth late one night last week at Mount Sinai South Nassau hospital.
Mixed with the joy of seeing their first child was an intense sadness and pain. He had tested positive for the coronavirus that morning, April 28, so he had to watch the birth alone from more than 20 miles away, on a smartphone screen.
“It hurts me so much,” Carchipulla said in Spanish from the couple’s home in Jackson Heights, Queens, as his newborn daughter, Danaey, cried a few feet from an iPad that a surgical technologist pointed toward Garcia in a labor and delivery room in Oceanside. “But thank God it all turned out well.”
This is a birth in the era of COVID-19. Parents are sometimes separated. Moms who test positive don masks before holding their babies. And there’s an empty waiting room where family and friends once gathered in anxious anticipation.
Newsday spent April 28 in the maternity unit of South Nassau to show how COVID-19 has changed the birthing experience for parents who carry the virus — one in four mothers at the hospital had tested positive at one point — and for those who don’t.
Watch the story
The coronavirus has taken more than 3,500 lives on Long Island since the first positive case was announced on March 5 in Nassau County. At the peak of COVID-19 hospitalizations in early April, coronavirus patients crowded emergency-room hallways, and some were triaged in outdoor tents.
South Nassau has tried to shield the maternity unit from the COVID-19 crisis that envelops most of the hospital. Designated elevators that are disinfected many times each day stop only at the maternity wing, to ease prospective parents’ fears of contagion. It’s easy to at least momentarily forget a lethal pandemic when a new life is born and a smiling nurse hands a crying newborn to an elated mother.
Yet most of the maternity unit at South Nassau is almost eerily peaceful.
“Before COVID, there would be a really festive environment,” said Dr. Alan Garely, the hospital’s chair of obstetrics and gynecology. “There’d be a lot of people, a lot of food, a lot of laughter, a lot of happiness. Now it’s strictly quiet and solitary.”
No visitors have been allowed except for a support person, usually the baby’s father.

Bradley Camhi is required to leave his wife, Becky, and newborn, Fredric, two hours after delivery at Mount Sinai South Nassau hospital on April 28. Credit: Jeffrey Basinger
Becky and Bradley Camhi of East Rockaway recalled how shortly after their first son, Jordan, was born two years ago, her parents and his mother were in the room celebrating, with aunts and uncles and cousins following not long after.
When son Fredric was born April 28, it was just him.
“It’s sad in a sense,” Bradley Camhi said.
Under a South Nassau rule aimed at limiting the spread of COVID-19, Bradley Camhi had to leave the hospital two hours after the birth.
That policy changed less than 24 hours later, when the state ordered all hospitals to allow a healthy primary support person to stay until the mother is discharged, and to permit doulas — trained birth coaches — in the labor and delivery room, if requested.
Family members talked with the Camhis by video after the birth, but, with social distancing, they won’t be able to see the baby even outside the hospital.
Becky Camhi, 31, said the grandparents are especially heartbroken. “It’s crushing them,” she said.
The families of Garcia and Carchipulla are in Ecuador, so after his coronavirus test came back positive, there was “no family member to accompany her” as she gave birth, Carchipulla said.
He was stunned that he had contracted the virus. Carchipulla, 32, said he quit his job as a manager and waiter at a Manhattan restaurant weeks ago, to limit his exposure to the virus, and he and his wife left home only to go to the supermarket, pharmacy or doctor’s office.
Asked as his wife was in labor how he felt being at home while she was about to give birth, he began to weep. “Very bad,” he said, putting his hands to his eyes and unable to utter another word.
A surgical technologist grabbed the iPad and brought it near the bed. Garcia was getting close to delivering.
“One more time: 1, 2, 3, 4, 5, 6, 7, 8, 9, 10,” the doctor, nurses and surgical technologists said in a chorus, asking Garcia to push.
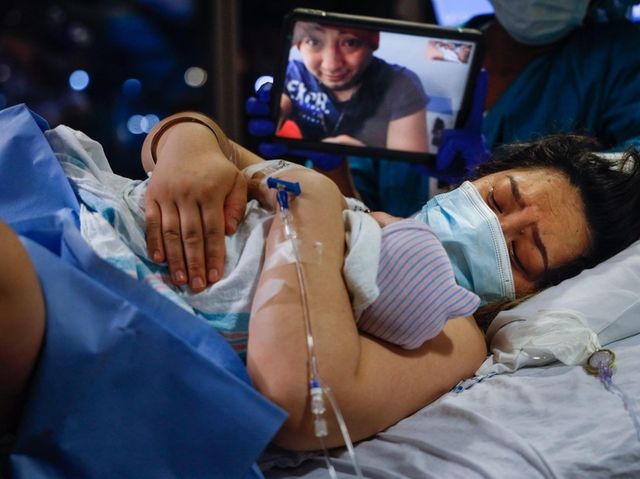
Manuel Carchipulla cries as he sees, via FaceTime, his wife hold their baby for the first time. Credit: Jeffrey Basinger

Diana Garcia Garcia holds Danaey, who was born at 10:35 p.m. April 28 and weighed 7 pounds, 4 ounces. Credit: Jeffrey Basinger
There was a collective cheer when the baby began to emerge. Garcia and, from a distance, Carchipulla, began to cry, and moments later, Danaey started to cry as well.
Soon after, Garcia, 31, pointed to the iPad and said to her daughter, “Look at Daddy.”
“Hello, my daughter,” he said, laughing through tears.
Danaey was born at 10:35 p.m., weighing 7 pounds, 4 ounces.
The surgical technologist let Carchipulla watch as the baby was cleaned and examined.
“Quiet, my love, quiet, don’t cry,” he said, a big smile on his face and tears in his eyes.
Garcia said the absence of her husband “hurts a lot.”
“A few hours ago, we were happy, preparing clothes for the baby,” she said in Spanish. “We didn’t expect this.”
On the morning of April 29, only hours after she gave birth, Garcia began to have a fever that rose to 100.5 degrees. She was tested again for the coronavirus. This time, she was positive.
Dr. Aaron Glatt, chairman of medicine and chief of infectious diseases at South Nassau, said it takes two to 14 days for the virus to show up on tests, so the two may have contracted the virus at about the same time, but, for whatever reason, Carchipulla tested positive before his wife.
Danaey tested negative, Carchipulla said, so, “for the safety of the baby,” when his wife and daughter were released from South Nassau on Friday, a distant cousin of Garcia’s picked up Danaey from the hospital and took her to Brooklyn to live with her until the couple tests negative. Carchipulla said he and Garcia are both now symptom-free.
After the positive test result, Danaey was placed in an incubator in Garcia’s hospital room.
Mothers who test positive are allowed to hold and breastfeed their newborns — the virus has not been detected in breast milk, according to the U.S. Centers for Disease Control and Prevention — but must wear masks and wash their hands regularly, said Elena Lobatch, South Nassau’s director of nursing for women and children’s services.
“A lot of hospitals still separate the mother and the baby” if the mother tests positive, Garely said. “But that’s not something we believe in, and we still advocate for the mother and for the bonding experience. We think that it’s part of child development. It’s a huge thing. There have been studies that show when mothers bond early with the babies, the relationship between the two sustains and is a stronger and better relationship.”
The hospital tries to balance the importance of that bond with the risk of transmission to the baby, he said. Children with COVID-19 generally have only mild symptoms, the CDC reports.

Manuel Carchipulla, who tested positive for COVID-19 and was not permitted to attend the birth of Danaey, cries while saying “te amo” to his daughter via FaceTime. Credit: Jeffrey Basinger
Keeping the baby from the mother also isn’t practical, Lobatch said.
“Realistically, when she is going home in 24 hours, who’s going to take care of this baby?” she asked. “Mom will. Will she be breast feeding if she wants to? Absolutely. So our philosophy is we will support her here. We’re better off teaching her or guiding her to exercise good hand hygiene, good isolation practices, so she can better adjust at home. It’s not like she’s going home and she’s handing the baby away to somebody to care for. It’s her and the partner.”
And, with COVID-19, there’s “no advantage of grandma stopping by or auntie stopping by or family friends stopping by and helping,” Lobatch said.
At home, as in the hospital, mothers with the virus are advised to limit contact with their newborns as much as possible, she said.
Transmission of the coronavirus from a mother to a baby is unlikely during pregnancy, and it has not been detected in maternal fluids, such as the amniotic fluid that surrounds the fetus, according to the CDC. A very small number of babies have tested positive shortly after they were born, but it’s not clear if the infants were infected before or after birth, the CDC says.
All mothers and their partners at South Nassau are tested for the coronavirus upon or before admission, and 18% of moms who have delivered since late March at the hospital have tested positive — down from 27% on April 13, a reflection of the success of social isolation efforts, Garely said.
Four of the women were seriously ill and required oxygen delivered through masks or nasal prongs, and their newborns were cared for in a separate room, Lobatch said. One of the women had such severe breathing problems that she was induced to go into labor at 34 weeks “to help her disease and to help the chances for the baby,” Garely said. The mother recovered after more than a week of treatment in the hospital, and the baby was healthy. The other mothers also recovered.
The rest have been asymptomatic or had only mild symptoms. Their babies were placed in the same room, but at least 6 feet away, and nurses made frequent rounds to check on them, said Patricia Bartels, nurse manager for labor and delivery.
The babies are tested 24 hours after birth, and 24 hours after that, if they’re still at the hospital, Garely said. If the baby is not in the hospital 48 hours later, the mother is asked to obtain a test for her baby at a pediatrician’s office. None of the newborns has tested positive, Garely said.
“It confirms the assumption that the virus is not transmitted through the placenta and the babies are born uninfected,” he said.
Partners who test positive have the same rules for contact with the baby as moms who test positive, including holding the baby only with a surgical mask covering the nose and mouth, Lobatch said.

Shannon Koledin, 28, was without her husband when their daughter, Mikaela, was born April 28 at Mount Sinai South Nassau hospital. Credit: Jeffrey Basinger

With family forced to stay away, Shannon Koledin looks over at Mikaela in her room at Mount Sinai South Nassau. Credit: Jeffrey Basinger
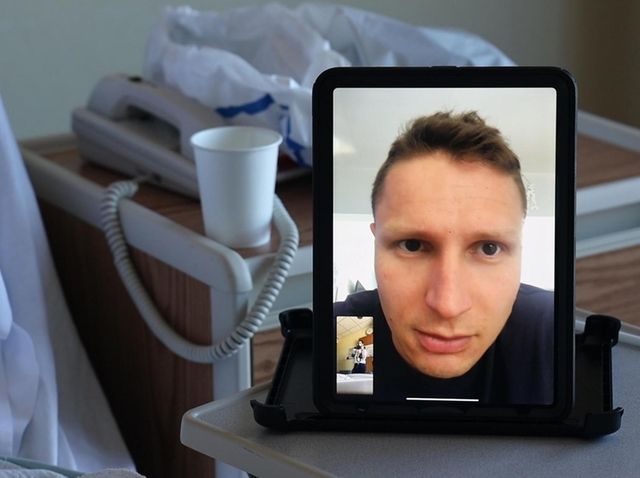
Michael Koledin, who tested positive for the coronavirus before Mikaela was born, sees his wife and newborn child on FaceTime on April 28. Credit: Jeffrey Basinger
Yet Michael Koledin, who tested positive for the coronavirus before his daughter, Mikaela, was born early April 28, was still wary and only held her briefly, with a mask and gloves, when she came home with his wife, Shannon, the next day.
“I’m definitely nervous about it,” he said. “There are a lot of unknowns about COVID-19.”
Koledin, 31, an FDNY firefighter in Queens, first tested positive on April 3. He had body aches and mild fever, but lately only a cough and mild headache were lingering, and it was getting better, making him assume he no longer carried the virus.
“When I found out he tested positive again, I think I cried for the rest of the night,” Shannon Koledin, 28, said.
Michael Koledin has been living in the den of the couple’s Massapequa home and will continue doing so until after he’s symptom-free.
During Mikaela’s birth, Shannon’s mother was with her, but “I just wanted that moment of when she was born to have him with me and to experience it together,” Shannon said. “It’s our first baby.”
Instead, he watched the birth on FaceTime.
A few hours later, Shannon lay in a quiet room that, she said, probably would have had a steady stream of family and friends visiting — along with Michael, of course, who instead was only an image on a computer screen.
Michael said the morning of his daughter’s birth, FaceTime “did make me feel like I was a part of the process and I was there for her. I don’t think it really took away from the moment. I still cried when I saw my daughter.”
He doesn’t dwell on not being able to kiss his newborn, or on how different it would have been if he hadn’t become a dad during a pandemic.
“It was such a joyful moment,” Michael said. “So I feel if I have regrets about it, it will take away from the joy.”
